In the last few days news
organizations reported an outbreak of Ebola in West Africa, leading (as of
March 24th) to a death of 59 out of 80 infected people.
The Ebola virus and its variant Marburg virus
are known to be one the most lethal viruses infecting humans. Once infected
patients die of hemorrhagic fever, a painful and agonizing death characterized
by fever, excessive blood loss and diarrhea.
There is no effective therapy,
except replacing fluids, blood, coagualnts as well as relatively generic measures
such as the administration of Immunoglobulin or antiviral pharmaceuticals such
as Ribavirin or S--adenosylhomocysteine (SAH) hydrolase
inhibitors. Antibiotics are also given to prevent secondary infections should
the patient survive. Novel treatments include the use of antisense RNA, which
has been shown to treat infections in non-human primates under experimental
conditions. The application of a recombinant vesicular stomatitis virus
expressing the Glycoprotein from Ebola has been developed as well and might
prevent death of the patient.
In order to prevent the infection from spreading
into the community, patients have to be quarantined and caregivers have to wear
protective clothing. The mortality is high, varying from 90% in the case of
Ebola Zaire to 34% to Ebola Bundibugyo; a special case might be Ebola
Reston, which did not cause any fatality among humans –although it is not clear
if humans can get infected in the first place.
The following strains of Ebola virus have been
identified during past epidemics:
- Ebola Zaire (1976)
- Ebola Sudan (1976)
- Ebola Côte d'Ivoire (1994; also known as Tai Forest Virus and may only be a close relative to Ebola)
- Ebola Reston (1994; causing simian hemorrhagic fever, not infectious for humans)
- Ebola Bundibugyo (2007)
A relative of Ebola, Marburg Virus (closely related to Ebola but distinct from) was identified in the
1960s to be the causative agent of a small epidemic of hemorrhagic fever among animal care workers in Marburg/Germany and Yugoslavia with a fatality rate of
23-90%.
In general the first symptoms of disease include a general malaise with Influenza-like symptoms, including fever/chills, chest pain, and phryngitis. If the central nervous is affected symptoms include severe headache, depression, confusion, fatigue, and coma. The most visible symptoms include hemorrhagic symptoms -
such as bleeding at injection sites, and hematomas. Death generally occurs because of low blood pressure,
tissue necrosis and multiple organ dysfunction.
Ebola and Marburg virus’ belong to the order of the
Mononegavirales -an order which includes other viruses of interest, Hendra and Nipah Virus, both which cause serious diseases in their own right- and the family of Filoviridiae.
 |
| Organisation of the Filovirus genome |
As such, the viruses have a negative strand RNA genome with a length of approximately 19kb, encoding for seven genes (NP, VP35,VP40,(s)GP, VP30, VP24 and L) each gene is flanked by a Non Translated (NTS) 3’ leader sequence and a 5’ trailer sequence (see figure), a feature shared with Nipah and Hendra viruses. Furthermore a non-coding region of varying length separates most genes. Five of the proteins encoded are shared with other negative ssRNA viruses (including the RNA dependent RNA Polymerase or L-protein and the Glycoprotein (GP)), whilst the Viral Proteins (VP) 35 and 40 are unique to Filoviruses.
Ebola viruses, similar to other Filoviridiae, infect not only human and non-human
primates but other animals such as pigs and some species of fruit bats as
well, in addition to a wide variety of cell lines. Cell types susceptible to Filovirus infection include but not limited to adrenal cortical cell, hepatocytes,
endothelial cells, fibroblasts, dendritic cells, monocytes, and macrophages, thus explaining
the wide range of symptoms in infected individuals.
Following exposure to both Ebola and Marburg virus, early targets of the virus include cells constituting the immune system -macrophages, dendritic cells and monocytes. This allows the virus to be spread to other parts of the body via the lymphatic and blood system, reaching the liver and the intestine. In addition, non-infected lymphocytes are depleted by probably via the induction of bystander apoptosis rather than infection with nascent virus.
Functions of the proteins
As mentioned above the L gene encodes the RNA
dependent RNA Polymerase that is required for the conversion of the negative
ssRNA into the positive strand RNA which serves as a template for negative ssRNA
(to be incorporated into the genome of newly synthesized viral particles) as
well as the synthesis of seven monocistronic mRNA species.
 |
| Simplified illustration of the Filovirus replication cycle |
The glycoprotein is incorporated into the membrane
of viral particles and –upon infection- binds to the receptor of the host cell,
whilst the function of the soluble Glycoprotein (which is secreted and not
incorpor-ated into the nucleocapsid and unique to Ebola virus) is unknown.
The Nucleocapsid (NP) and VP 35/24 proteins are required for
the assembly of the viral particle whereas VP 30 is required for viral budding
– the release of the virus particle from the host cell. In addition of its
function in the assembly of the viral particle the Nucleocapsid protein might
also be involved in the transport of the pre-assembled particle to the surface
of the infected cell along the microtubuli. Prior to its incorporation in the
virus particle the Glycoprotein is modified within the Golgi.
Because of the mortality of Ebola and Ebola related viruses,
outbreaks are self limiting and relatively small in terms of numbers of people
infected. The virus is also mostly transmitted by close contact with infected
patients in addition to poor sanitary conditions and contaminated water and
food. The virus is believed to have originally been limited to infect primates
and fruit bats – although the natural host has not been identified with
absolute certainty. It crossed the species barrier only when humans started to
explore those areas. Ebola and Ebola-related diseases are considered to be
zoonotic –of animal origin. In the case of
Ebola, larger epidemics have been avoided so far, probably thanks to the
high mortality this virus exhibits.
Interactions between viral proteins and the host cell
In recent years detailed analysis has revealed a number of cellular proteins which are interacting with different viral proteins during the infectious cycle of Ebola virus.

Most notably this work has identified not only the cellular receptors required for viral entry but also proteins required for the release of the viral genome into the cytoplasm of the host cell. As it turns out both the fusion of Filoviruses and the release of the genome into the cytoplasm closely resemble the mechanism found in Influenza virus and other pathogens. It should be noted that there is no bona fide receptor for Ebola or Marburg virus, but it seems that some might function as co-receptor or that the virus can bind different receptors. Viral entry itself is mediated by lipid raft dependent mechanisms and macropinocytes, a specialized subtype of endocytosis. Following entry into the cytoplasm, the viral genome is released in a Cathepsin B and L dependent process similar to the release of the Influenza virus genome, although this varies between cell lines (in Vero cells, Cathepsin L is required but is dispensable in human dendritic cells).
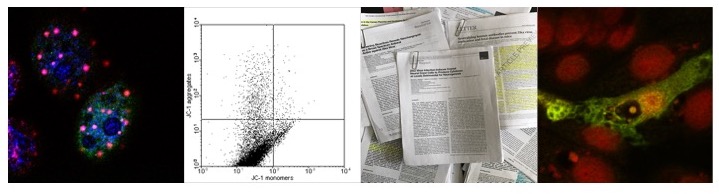
Studies using different cell lines confirmed the presence of a clear cytopathic effect (CPE) , although with a different severity which depends not only on the virus but also on the cell line used. Interestingly primary human cells -macrovascular or microvascular endothelial cells as well as macrophages and monocytes derived from normal peripheral blood -infected with Ebola do not exhibit any CPE. Cell death of other cell types infected -such as hepatocytes- seems to be non-apototic although Ebola virus does not antagonize apoptotic signaling pathways.
More recent results enabled to visualize the formation of nascent viral particles in distinct inclusion bodies by live cell microscopy. In theory it might be possible now to almost observe viral infection "live as it happens", thus leading to new insights into the biology and pathogenesis of diseases caused by Filoviruses.
Further reading:
Mühlberger E (2007). Filovirus replication and transcription. Future virology, 2 (2), 205-215 PMID: 24093048
Huggins, J., Zhang, Z., & Bray, M. (1999). Antiviral Drug Therapy of Filovirus Infections: S‐Adenosylhomocysteine Hydrolase Inhibitors Inhibit Ebola Virus In Vitro and in a Lethal Mouse Model The Journal of Infectious Diseases, 179 (s1) DOI: 10.1086/514316 Takada A (2012). Filovirus tropism: cellular molecules for viral entry. Frontiers in microbiology, 3 PMID: 22363323
Kiley MP, Bowen ET, Eddy GA, Isaäcson M, Johnson KM, McCormick JB, Murphy FA, Pattyn SR, Peters D, Prozesky OW, Regnery RL, Simpson DI, Slenczka W, Sureau P, van der Groen G, Webb PA, & Wulff H (1982). Filoviridae: a taxonomic home for Marburg and Ebola viruses? Intervirology, 18 (1-2), 24-32 PMID: 7118520
Nanbo A, Watanabe S, Halfmann P, & Kawaoka Y (2013). The spatio-temporal distribution dynamics of Ebola virus proteins and RNA in infected cells. Scientific reports, 3 PMID: 23383374
Hoenen T, Shabman RS, Groseth A, Herwig A, Weber M, Schudt G, Dolnik O, Basler CF, Becker S, & Feldmann H (2012). Inclusion bodies are a site of ebolavirus replication. Journal of virology, 86 (21), 11779-88 PMID: 22915810
Iwasa A, Halfmann P, Noda T, Oyama M, Kozuka-Hata H, Watanabe S, Shimojima M, Watanabe T, & Kawaoka Y (2011). Contribution of Sec61α to the life cycle of Ebola virus. The Journal of infectious diseases, 204 Suppl 3 PMID: 21987770
Hofmann-Winkler H, Kaup F, & Pöhlmann S (2012). Host cell factors in filovirus entry: novel players, new insights. Viruses, 4 (12), 3336-62 PMID: 23342362
Sayama Y, Demetria C, Saito M, Azul RR, Taniguchi S, Fukushi S, Yoshikawa T, Iizuka I, Mizutani T, Kurane I, Malbas FF Jr, Lupisan S, Catbagan DP, Animas SB, Morales RG, Lopez EL, Dazo KR, Cruz MS, Olveda R, Saijo M, Oshitani H, & Morikawa S (2012). A seroepidemiologic study of Reston ebolavirus in swine in the Philippines. BMC veterinary research, 8 PMID: 22709971
Greetings, I linked your blog to twitter and one of my followers @stgoldst (PhD student of virology) mentioned some clarifications. He mentioned that Marburg and Ebola aren't 'related' nor is Marburg a prototype of Ebola. Per: "The prototype of Ebola, Marburg Virus (closely related to Ebola but distinct from)..." Though they are in the same family of viruses they are quite different species on a similar level as SARS and MERS was his comparison; so I guess it just depends on what you define as closely related. Perhaps it's just more accurate to say they are in the same viral family and cause similar symptoms perhaps? Relatedness might have suggested genetics and they are actually quite different genetically. And you mentioned: "Ebola Reston (1994; Simian Hemorrhagic Fever Virus, not infectious for humans)", he said simian hemorrhagic fever virus is in a different viral family from Ebola Reston...Arteriviridae. Did you mean that Ebola was also discovered in 1994 during an SHFV outbreak? Just thought I'd toss in some thoughts, I work on Flavis...but I've only started working the infectious disease field since 2010, prior to that I was microbial/viral ecology (environmental, not health related). Cheers. Feel free to chat up @stgoldst on twitter if you want :)
ReplyDeleteDear Mel,
DeleteThanks for your comment.
You are correct in your statement that Simian hemorrhagic fever virus is a positive strand RNA virus belonging to the Arteriviridae within the order of the Nidovirales – but Ebola Reston is (in contrast to the other Ebola viruses) the causative agent of simian hemorrhagic fever. It is a case where a different virus causes a similar disease (similar in the symptoms). According to Dalgard et al. (1992) and Fischer- Hoch et al. (1992) both viruses (Ebola Reston and SHFV) were isolated during the outbreak at the animal facility in Reston and it was only in subsequent laboratory studies that Ebola Reston was shown to be highly pathogenic for monkeys. Ebola Reston was also postulated to have infected swine in the Philippines in 2008, so it seems that (similar to other Ebola viruses) not only infects monkeys but swine as well (Sayama et al., 2013).
Regarding the closeness of both Marburg and Ebola, so it seems that it partly depends on the sequence of individual genes on the definition of closeness. From an antigenic point of view both are certainly cousins, and hence are classified in different genera. This is different from MERS-CoV and SARS-CoV, where both are of the same genus (Betacoronavirus) but of different lineages (de Groot et al., 2013)
You might find that I decided to clarify these points in my post. I hope this anwers your questions.
Never give up in life they all say no cure to HSV 2 which is a big lie I have pass through many process also i never believe there is really cure to HERPES until I meet Dr.Emmanuel the doctor that have been helping many people for many years, I come across this doctor online when I was searching for cure online I found out about this man, and to my greatest surprise this man have the herbal medicine which I have been looking for years I explain my problem to him through the email I found on someone who testify about him also, Dr.Emmanuel write me a reply and explain how the process work so after ordering for the medicine I got it within 4 days and I took it according to the way Dr.Emmanuel instructed, I was so happy after two week I took the medicine there was very big change in my health when I was done with the process I go for test, I found out I am negative that was the day I have the tears of joy you can also get in contact with my doctor through his email now nativehealthclinic@gmail.com or you can also WhatsApp him +2348140073965. And He a lso have herbs medicine to cured the following diseases; eczema,urethra wart,chronic problems.Herpes, Cancer, Als,Hepatitis, Diabetes, HPV,Infections,ulcer ETC
DeleteI want to write a little testimony about the good work of doctor ehiaguna who cured me from Hsv 1 and 2 for just 2 week with his herbal medicine, I never believe I can be normal again and have a good life like others I always regretted the day I got diagnose with the virus, I was lost of hope when my doctor told me there is no cure for it but I keep thinking and thinking about my future, if I can have kids of my own well I am so grateful for my helper who get me cured with his herbal medicine, I go online in search of anything that can help me because I can’t deal with it forever so I found this doc ehiaguna email on a blog of someone who was cured by him I quickly contact him for help and explain all my pain to him, he told me not to worry about it there is cure for real, I never believe until he send me the herbal medicine when I order for it and I have it within 4 days that is how I took the medicine for 2 week and the following week I go for test just to confirm I was 100% cured from this sickness what a miracle in my life I am so happy right now, you can also get in contact with him if you have such sickness through drehiaguna@gmail.com and also WhatsApp him +2348073908953... And He also have herbs medicine to cured the following diseases; eczema,urethra wart,chronic problems.Herpes, Cancer, Als,Hepatitis, Diabetes, HPV,Infections,ulcer ETC
DeleteI’m recommending Dr Godday to everyone who have herpes virus to get the cure from him. I was diagnose of genital herpes in 2015 and i have been searching and asking questions to see if i could get something to cure the disease because i did not believe what the doctors say that no cure is found yet. I came across a comment on Youtube and the person testify how she was cured from herpes and hpv after using Dr Godday herbal medicine. I quickly contact Dr email and explain my problem to him and he prepare the herbs and send it to me through courier and gave me instructions on how to use it and tell me to go for checkup after usage which i did after two weeks of taken the herbal medicine and my result was NEGATIVE. I waited another month and retested the result was still NEGATIVE and my doctor told me that am completely free from herpes. Am so happy and grateful to Dr Godday for what he has done for me and i will continue to share this for people out there to know that there is cure for herpes. You can contact Dr Godday on email and WhatsApp to get the cure from him. Email:goddayspiritualhome@gmail.com Or Call/What’s-app +1{919}4956404
Delete2 WEEKS AGO I ENDED NATURAL HERBAL TREATMENT FROM TRADITIONAL HEALER WHO IS IN AFRICAN, I GOT RID OF HPV VIRUS OUT OF MY BODY WITH HIS HERBAL TREATMENT. It SO AMAZING I'M FREE FROM THIS VIRUS FOREVER. YOU CAN REACH HIM ON; DRONOKUNHERBALCURE@GMAIL.COM
ReplyDeleteMY LIFE IS BACK, Am so happy to share this testimony on how Dr LUCKY , was able to heal me from HpV Disease, well i was detected positive on 23th may 2015, and ever since i have been looking for a way to treat and cure this disease from me, but all ways i try there was no solution, few weeks ago i saw a testimony of some people on how Dr LUCKY was able to cure them from HpV disease, still on i heard about it on media when a young lady also gave her testimony about this same Dr, well left with no hope i message Dr LUCKY , telling him all my problem, he told me what we were to do, that he was going to send me a portion which i am going to take, and after which i took this herb portion he sent to me, he told me to go back to the hospital for check up and after i have done that i should come and tell him the good news result, at first when i saw the message i was so shock and still did not believed i will be cured, well friend to make my story short i am HpV negative now after many time of sorrow, i am Negative, and my sickness are gone, i thank God for leading me to this man….you can email him on (drluckyherbalcure@gmail.com) or you can also call him +2348154637647, he can be of help to you on any problem like
ReplyDelete{1} HIV/AIDS
{2CANCER
{3}HERPES
{4}DIABETES
(5}HERPERTITIS B
(6)PID Virus.
MY LIFE IS BACK, Am so happy to share this testimony on how Dr LUCKY , was able to heal me from HpV Disease, well i was detected positive on 23th may 2015, and ever since i have been looking for a way to treat and cure this disease from me, but all ways i try there was no solution, few weeks ago i saw a testimony of some people on how Dr LUCKY was able to cure them from HpV disease, still on i heard about it on media when a young lady also gave her testimony about this same Dr, well left with no hope i message Dr LUCKY , telling him all my problem, he told me what we were to do, that he was going to send me a portion which i am going to take, and after which i took this herb portion he sent to me, he told me to go back to the hospital for check up and after i have done that i should come and tell him the good news result, at first when i saw the message i was so shock and still did not believed i will be cured, well friend to make my story short i am HpV negative now after many time of sorrow, i am Negative, and my sickness are gone, i thank God for leading me to this man….you can email him on (drluckyherbalcure@gmail.com) or you can also call him +2348154637647, he can be of help to you on any problem like
ReplyDelete{1} HIV/AIDS
{2CANCER
{3}HERPES
{4}DIABETES
(5}HERPERTITIS B
(6)PID Virus.
I has suffered for Human papillomavirus (HPV) for 2years, I was given some tablets at the hospital but I refused to take it, They said I have to be on it for life so I don't want take a drugs everyday for life. No point in taking medicine everyday when u won't get cure from it and I was advice to seek for natural herbal cure, after some time I found dr uza is the most trustful herbalist that have herbs to cure wicked symptom's,I emailed dr uza, for 2weeks been his patient he cured my (HPV) with his herbal. I only used his natural herbs for two weeks it was 100% cure. I'm not (HPV) patient anymore. I'm happy about it i finally got cured out of this mess been in my body for 2years. I also recommend you if you're living with (HPV) or herpes symptoms i also want you to be free contact dr uza with the email attach to my post. druzaherbalcure@gmail.com
ReplyDeleteI has suffered for Human papillomavirus (HPV) for 2years, I was given some tablets at the hospital but I refused to take it, They said I have to be on it for life so I don't want take a drugs everyday for life. No point in taking medicine everyday when u won't get cure from it and I was advice to seek for natural herbal cure, after some time I found dr uza is the most trustful herbalist that have herbs to cure wicked symptom's,I emailed dr uza, for 2weeks been his patient he cured my (HPV) with his herbal. I only used his natural herbs for two weeks it was 100% cure. I'm not (HPV) patient anymore. I'm happy about it i finally got cured out of this mess been in my body for 2years. I also recommend you if you're living with (HPV) or herpes symptoms i also want you to be free contact dr uza with the email attach to my post. druzaherbalcure@gmail.com
ReplyDeleteI am so happy, i never believe i will be this happy again in life, I was working as an air-hoster ( cabby crew ) for 3years but early this year, i loose my job because of this deadly disease called Herpes virus (HSV), I never felt sick or have any symptom, till all workers were ask to bring their doctors report, that was how i got tested and i found out that am HSV positive that make me loose my job, because it was consider as an STD and is incurable disease, i was so depress was thinking of committing suicide, till i explain to a friend of mine, who always said to me a problem share is a problem solved, that was how she directed me to Dr Isibor, that was how i contacted him and get the medication from this doctor and i got cured for real, I just went back to my work and they also carry out the test to be real sure and i was negative. Please contact this doctor if you are herpes positive diseases his email is: drisiborspellhome@gmail.com. or you can call or whatsApp his mobile number +2348107855231.
ReplyDeleteI was diagnose with human papilloma virus (HPV) 4 years ago and i met a doctor he told me there is no cure and i have be taking some medication the warts multiplied when trying to removed them and it got me embarrass and pains, luckily few weeks ago i was recommend to Dr Onokun for natural treatment after one week i got 100% cure and all the wart and pains got disappeared, i sheared this post because its part of my life experience, encase anyone need speedy help about this cure email Dr Onokun via, dronokunherbalcure@gmail.com
ReplyDeleteJust got diagnosed with HSV1, and reading this actually made me feel like crawling and crying like a baby. The outbreak I have right now is genital and in my throat and mouth, I talked to the doctor who did the blood test on me and said over time that it would eventually get much better. She said that what I’m having is a massive outbreak and is unusual, but that it may be due to the fact that I stressed myself out over it so much. She also told me even though I have it in the genital area that It doesn't mean that I needed “private to private” contact to acquire it. But this did make me feel a whole lot better about the whole situation. For anyone else to have HSV1 after all this stress and pains am passing and the doctor saying all such of crap i was not convince by his Theory so i decided to go on the internet and saw this comments by Rose who testify about how she get cured by root and herbs by Chief Dr Wealthy, when i first bump into it i didn't believe the comments at first so i decided to confront her on Facebook and really know what and how did it work because my doctor told me there is no cure for herpes, so i really contacted Chief Dr Wealthy, he responded in A minute the only thing he ever ask for was just the items of which he will use to prepare for the herbs, after all this he send the herbs through courier Services, within 2 week i was cure just like that without no struggle or stress, if you are out there in need of cure contact him with his email address: wealthylovespell@gmail.com or you Whatsapp him.+2348105150446
ReplyDeleteHello everyone, I was infected with the Epstein-Barr virus and I got cured from the Epstein-Barr virus few months ago after i contacted Chief Dr Wealthy. I saw a post on the internet after i have seek healing for several years from different doctors in California. I sent the Doctor a request for help, just a few email i followed his instruction and he sent me the medication. Now i am negative and i referred him to all my friend who had this same sickness and they have gotten their cure too. You can contact him via his email: wealthylovespell@gmail.com or Phone call or whatsAPP: +2348105150446. While i was on his medication i understood that he can also cure HERPES, HIV/AIDS, CANCER, Male/female menopause, Miscarriage, Menstruation problems, PREGNANCY PROBLEM, EPILEPSY, GONORRHEA, LASSA FEVER, OBESITY, KIDNEY FAILURE, HYPERTENSION, FIBROID TUMOR, BRAIN FOG, EPSTEIN-BARR VIRUS and many more.
ReplyDeleteContact him today and get your problem solved.
I'm 61 years old, I contracted hpv in 2011' I has be taking lot treatment for it and some months ago the wart stated coming out seriously, I used lot recommendation because there was lot warts around my anus and was so embarrassed. but today I'm totally happy I got the virus eliminated by using natural treatment from Dr Onokun herbal center after his treatment I got cured. all the warts went away' seriously believed Dr Onokun he have the cure for human papillomavirus because he has eliminated hpv been in my body since 2011, Dr Onokun make it possible for me. Here is Dr Onokun email to reach him: Dronokunherbalcure@gmail.com he is welled capable of curing terrible diseases.
ReplyDeleteI'm 61 years old, I contracted hpv in 2011' I has be taking lot treatment for it and embarrassedsome months ago the wart stated coming out seriously, I used lot recommendation because there was lot warts around my anus and was so . but today I'm totally happy I got the virus eliminated by using natural treatment from Dr Onokun herbal center after his treatment I got cured. all the warts went away' seriously believed Dr Onokun he have the cure for human papillomavirus because he has eliminated hpv been in my body since 2011, Dr Onokun make it possible for me. Here is Dr Onokun email to reach him: Dronokunherbalcure@gmail.com he is welled capable of curing terrible diseases.
ReplyDeleteThis is really serious, who will believe that a herb can cure herpes, i never believe that this will work, i have spend a lot getting drugs from the hospital to keep me healthy, it got to a time that i was waiting for death to come because i was broke, one day i hard about this great man called Dr Azaka who is well know for Herpes, HIV and Cancer cure, i decided to email him I didn't believe him that much, I just wanted to give him a try, he replied my mail and Needed some Information about me, then I sent them to him, he prepared a herbal medicine (CURE) and sent it through Online Courier Service for delivery, he gave my details to the Courier Office. they told me that 3-5 days I will receive the package and after receiving it, i took the medicine as prescribed by him at the end of the one week, he told me to go to the hospital for a check up, and i went, surprising, after the test the doctor confirm me Herpes simplex virus negative, i thought it was a joke, i went to other hospital and was also negative, thank you for saving my life, I promise I will always testify of your good works. if you are herpes simplex virus patient, OR you are be helping by someone before i will like to advice you to give this man a tryand see what will happen to your life don't worry about the money you have being using contact him and I am sure you, you will get cured, WhatsApp him on +2349059389105 or email via drazakaojezele@gmail.com Dr Azaka IS ALSO SPECIALISED ON(1) CANCER,(2) DIABETES,(3) HIV&AIDS,(4) URINARY TRACT INFECTION,(5) FIBROID,(6) IMPOTENCE,(7) BARENESS/INFERTILITY,(8) PREGNANCY,
ReplyDeletemy husband and I have been married for about 7 yrs now. We were happily married with two kids, a boy and a girl. 3 months ago, I started to notice some strange behavior from him and a few weeks later I found out that my husband is seeing someone. He started coming home late from work, he hardly care about me or the kids anymore, Sometimes he goes out and doesn't even come back home for about 2-3 days. I did all I could to rectify this problem but all to no avail. I became very worried and needed help. As I was browsing through the Internet one day, I came across a website that suggested that Dr jeffrey can help solve marital problems, restore broken relationships and so on. So, I felt I should give him a try. I contacted him and he did a spell for me. Two days later, my husband came to me and apologized for the wrongs he did and promise never to do it again. Ever since then, everything has returned back to normal. I and my family are living together happily again.. All thanks to Dr jeffrey . If you need a spell caster that can cast a spell that truly works, I suggest you contact him. He will not disappoint you. This is his E-mail:
ReplyDeletedctrjeffrey@gmail.com
WhatsApp +2348162061202
i got hpv from my boyfriend and i was trying all i could do to get rid of this virus over 4 months now i have taking a lot of drugs from different medical doctor which didn't work at all, last month i was doing some research on google on how to get cured totally from this virus i found someone testimony on how she got cured totally from hpv with the help of doc. onokun natural herbs and she drop doc onokun email address, So i decide to give him a try and i contact him for help he told how to purchase the natural herbs and i did that, Do you believe i only took this herbs for 2 weeks and i got cured permanently from the hpv virus without no side effect. Thank you so much doc onokun for the help i will make sure i tell the whole world about you. contact him if you need his help too via: Dronokunherbalcure@gmail.com
ReplyDeleteI am really happy that i have been cured from (HERPES SIMPLEX VIRUS) with the herbal medicine of Dr OSAGIE , i have been suffering from this disease for the past 3 years and 4 mouth without solution until i came across the email of this doctor who have cure so many people with his herbal medicine, i also choose to give him a chance to help me and my husband, he told me what to do and i kindly did it, and he gave us his herbal medicine and direct me on how to use it, i also follow his instructions for use and he ask us to go for a check up after 1 week and 5days which i did, to my greatest surprise our result came out as negative, we are really happy that there is someone like this doctor who is ready to help anytime any day. To all the readers and viewers that is doubting this testimony stop doubting it and contact this doctor if you really have one and see if he will not actually help you. i am not a stupid woman that i will come out to the public and start saying what someone have not done for me and i know that there are some people out there who are really suffering and hurting their family just because of these diseases so you can to mail him on drosagiesolutiontemple@gmail.com OR
ReplyDeleteDROSAGIESOULTIONTEMPLE@YAHOO.COM or WHATSAPP +2347030465649 he also told me that he has cure for these diseases listed below .
HERPES SIMPLEX VIRUS.
.DIABETES .
CANCER
.HEPATITIS
.HIV/AIDS
Thank you for your time
My name is Giovanni, am feeling so much better now after Dr. Raymond healed me of corona virus with the help of a spell. it really hurt to have lost my mother and wife to this virus before meeting this great healer, i am so happy to have survive this deadly virus. A friend of mine Lee from China told me how this great Dr. Raymond healed two of his Daughter with a spell, so I decided to contact him immediately for help. I did as he instructed and now am healed completely. What a magnificent experience with Dr Raymond. I will not stop sharing these testimonies until each patients recovered. Thanks to the great Dr. Raymond for restoring my health. Contact him via: Email> swiftspellcast@gmail.com WhatsApp> +2348118116281
ReplyDeleteHe also solve issues listed below
(1)HIV/AIDS
(2) Herpes virus
(3) Do you want to be promoted in the office?
(4) Spiritual protection
(5) Do you want children?
(6) Do you want to get rich?
(7) You want your husband / wife to be yours forever?
(8) Do you need financial assistance?
(9) Are you cheated and want to Recover lost money?
(10) Cancer treatment and various diseases
(11) You want to stop divorce
(12) Commercial protection
(13) Looking for a job
(14) Body care
(15) Divorce spell. (16)Bring back my Ex.
If you need to resolve any of these issues today, please contact the solution temple ...
I was suffering from chronic hepatitis B , I spent alot on drugs, i never thought that a day like this will come and i will be able to give up on drugs. i found dr_anuge contact on blog when someone talked about DR ANUGE, so i contacted him via email: dranuge@gmail.com and made purchase of the hepatitis Vaccine, i received his herbal medicine through UPS delivery service within 3 days, when i received the medicine i applied it as prescribed and i was totally cured of hepatitis b within few's weeks of usages, i went back to my doctor and he confirmed i was free curable cured from the disease, am so happy now living a normal life again thanks to Dr_Anuge Viewers contact Him via email: dranuge@gmail.com Or you can also reach him via WhatsApp +2348164866838 He's also specialized in the following:HIV /AIDS CURE
ReplyDeleteHEPATITIS CURE
DIABETES CURE
STROKE
HERPES SIMPLEX CURE
EPILEPSY CANCER CURE
FIBROID
HIGH BLOOD PRESSURE
HERBAL MEDICINE FOR PREGNANCY
LOVE SPELL AND MONEY SPELL...
Never give up in life they all say no cure to HSV 2 which is a big lie I have pass through many process also i never believe there is really cure to HERPES until I meet Dr.Emmanuel the doctor that have been helping many people for many years, I come across this doctor online when I was searching for cure online I found out about this man, and to my greatest surprise this man have the herbal medicine which I have been looking for years I explain my problem to him through the email I found on someone who testify about him also, Dr.Emmanuel write me a reply and explain how the process work so after ordering for the medicine I got it within 4 days and I took it according to the way Dr.Emmanuel instructed, I was so happy after two week I took the medicine there was very big change in my health when I was done with the process I go for test, I found out I am negative that was the day I have the tears of joy you can also get in contact with my doctor through his email now nativehealthclinic@gmail.com or you can also WhatsApp him +2348140073965. And He a lso have herbs medicine to cured the following diseases; eczema,urethra wart,chronic problems.Herpes, Cancer, Als,Hepatitis, Diabetes, HPV,Infections,ulcer ETC
ReplyDeleteI want to write a little testimony about the good work of doctor ehiaguna who cured me from Hsv 1 and 2 for just 2 week with his herbal medicine, I never believe I can be normal again and have a good life like others I always regretted the day I got diagnose with the virus, I was lost of hope when my doctor told me there is no cure for it but I keep thinking and thinking about my future, if I can have kids of my own well I am so grateful for my helper who get me cured with his herbal medicine, I go online in search of anything that can help me because I can’t deal with it forever so I found this doc ehiaguna email on a blog of someone who was cured by him I quickly contact him for help and explain all my pain to him, he told me not to worry about it there is cure for real, I never believe until he send me the herbal medicine when I order for it and I have it within 4 days that is how I took the medicine for 2 week and the following week I go for test just to confirm I was 100% cured from this sickness what a miracle in my life I am so happy right now, you can also get in contact with him if you have such sickness through drehiaguna@gmail.com and also WhatsApp him +2348073908953... And He also have herbs medicine to cured the following diseases; eczema,urethra wart,chronic problems.Herpes, Cancer, Als,Hepatitis, Diabetes, HPV,Infections,ulcer ETC
ReplyDeleteI want to appreciate Dr Ehizele for using his herbal medicine to cure my family herpes virus,since 3years ago my family have been having this herpes disease and it have been giving my family challenges,we were so perplexed cause my family have taken several drugs to be cure but every of our effort was in-vain,a fateful morning i was browsing through the internet then i saw several testimonies about Dr.Ehizele curing people of their herpes disease immediately i contacted Dr Ehizele on his email: ehizeleherbalhome@gmail.com}, told him about my family troubles and he told me that my family must be cure,so he prepare a herbal medicine for my family which we use for 2 weeks and everything was like a dream for my family,my family herpes disease was totally gone. he an also cure the following, High/low blood pressure, HSV, 1,2 and 3, Diabetes, Cancer, Asthma Unable to get pregnant, heart problem, bad breath etc. why don't you contact him today and be free from your diseases on email, ehizeleherbalhome@gmail.com or whatsapp him on +2347089384319
ReplyDeleteGod bless Dr Ebacol for his marvelous work in my life, I was diagnosed of HERPES since 2018 and I was taking my medications, I wasn't satisfied i needed to get the HERPES out of my system,I searched out some possible cure for HERPES i saw a comment about Dr Ebacol, how he cured HERPES,DIABETES,HIV,and CANCER with his herbal medicine, I contacted him and he guided me. I asked for solutions, he started the remedy for my health, he sent me the medicine I took the medicine as prescribed by him and 14 days later i was cured from HERPES, Dr Ebacol truly you are great, do you need his help also? Why don’t you contact him through his EMAIL: drebacolherbalhome1@gmail.com call or whatsApp him on +2348159042641
ReplyDelete